Macular Degeneration Overview:
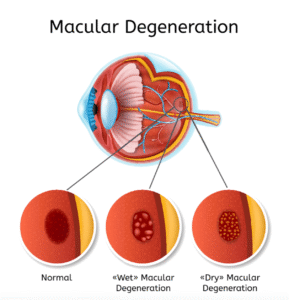
Macular degeneration is a disease of the macula, an area of the retina at the back of the eye that is responsible for fine detail vision. It is a common disease that appears in older adults and is the leading cause of vision loss in patients over 50. Vision loss usually occurs gradually and typically affects both eyes at different rates. Even with a loss of central vision, however, color vision and peripheral vision may remain clear.
SCHEDULE AN APPOINTMENT
If you would like to learn more about Macular Degeneration in Stockton, Modesto, & Manteca, CA call +1 (209) 239-5303 to make an appointment at Central Valley Eye Medical Group.
FAQ
There are two forms of age-related macular degeneration. The first type is dry macular degeneration, also known as non-neovascular. The second type is wet macular degeneration, also known as neovascular.
The root causes of macular degeneration are still unknown. However, it is more common in women and patients with light skin or eye color. Patients can minimize their risk by exercising, eating food rich in Omega-3 fatty acids, and seeing Central Valley Eye Medical Group for regular eye examinations. The following genetic and environmental factors can increase the risk of developing macular degeneration.
- Age: the majority of patients are over 65 years of age.
- Heredity: is common in some families but not in others
- Long-term sun exposure
- Smoking
- High blood pressure
- High cholesterol
- Hypertension
- Nutritional deficiencies
- Diabetes
- Head injury
- Infection
Dry macular degeneration can cause little, if any, change in vision. As the disease progresses, patients can experience difficulty seeing while reading or driving, the inability to see fine details, and develop blind spots in the center of vision. Additionally, patients can experience the feeling that objects “jump” when they try to look at them and objects can appear distorted, blurred, or abnormal in shape, size, and color. If the disease progresses to the wet form, patients can begin to perceive straight lines as wavy or crooked, have larger blind spots, and increased central vision loss. With wet macular degeneration, it can take as little as a few days or weeks for central vision loss to progress. Due to these symptoms, many patients require lifestyle changes. Patients can lose the ability to drive, read, or recognize faces. However, peripheral vision remains so patients typically remain capable of being independent.
At Central Valley Eye Medical Group, our doctors can identify changes of the macula during a routine eye examination. Even at the early stages and without symptoms we can identify macular degeneration by looking into your eyes with various instruments. We also use a chart known as an Amsler Grid which can pick up subtle changes in vision. Our staff also uses an angiography which is the most widely used macular degeneration diagnostic test. During the test, one of our doctors will inject a harmless orange-red dye, Fluorescein, into a vein in the arm. The dye travels through the body to the blood vessels in the retina. A special camera takes multiple photographs. The pictures are then analyzed to identify damage to the lining of the retina or atypical new blood vessels. The formation of new blood vessels from blood vessels in and under the macula is often the first physical sign that macular degeneration may develop. In addition, our staff has invested in an optical coherence tomography scanner which uses light waves to create a contour map of the retina and can show areas of thickening or fluid accumulation.
In addition to certain underlying diseases like hypertension, other risk factors for the development of macular degeneration include:
- Family history.
- Being over the age of 50.
- Smoking.
- A high-saturated diet.
While the symptoms may vary between patients, some of the most common ones include:
- Blurry vision
- Trouble recognizing faces of friends and family.
- Decrease of central vision line, which is needed for driving or reading close up.
In addition to a comprehensive eye exam, your physician may also perform the following diagnostic tests:
- Pupil dilation: Dilating your pupils allows for better visualization of your retina.
- Visual acuity testing: This type of testing gauges how well you can see at different distances.
- Angiography: Using fluorescein, which is a dye that can enhance the blood flow through your blood vessels and retina, pictures are taken, and your retina is then examined to look for signs of macular degeneration.
Treatment for macular degeneration depends on several factors:
- Your age and overall health.
- Your medical history.
- Medications you are currently taking.
- The severity of degeneration and your tolerance to treatment.
Schedule a Consultation
Seeking macular degeneration treatment in Stockton, CA or Manteca, CA?
Give us a call at +1 (209) 239-5303 or click here to fill out a contact form!