The diagnosis of glaucoma can often be nuanced and requires meticulous attention to detail over time. Given that glaucoma is a progressive condition, there are situations where the diagnosis will not be possible until your doctor has had time to follow you over time. Typically in this situation, your doctor will identify you as a “glaucoma suspect” and follow you closely to ensure you are treated if you show any clear signs of glaucoma in the future.
Alternatively, there are cases where glaucoma can be clearly identified and needs to be treated more urgently. Given that glaucoma typically does not cause any symptoms, everyone should get routine yearly comprehensive eye examinations starting at age 40. Prior to this, we recommend healthy individuals without any visual complaints get a full eye examination every 2-4 years, outside the standard age-appropriate eye health and vision screenings.
Diagnosing Glaucoma
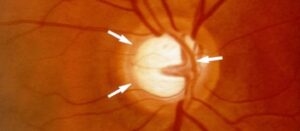
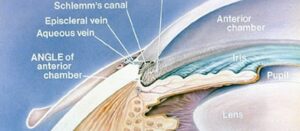
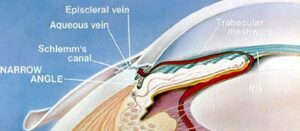
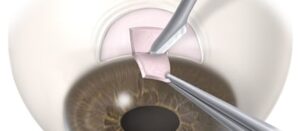
A glaucoma evaluation typically takes several hours and includes various glaucoma diagnostic tests, including an eye pressure check, a visual field test, an optic nerve imaging study, and a corneal thickness measurement. This is typically paired with a gonioscopic evaluation of the “angle” of the eye and a full dilated funduscopic examination to evaluate the optic nerve and the entire eye.
Initial treatment for glaucoma typically involves the use of medicated eye drops that help to lower eye pressure. In later-stage glaucoma, patients may need laser treatment or even surgery to help control their eye pressure.

See What Patients Had To Say!
“This place was great! As a new patient, I had minimal paperwork to fill out and the wait time was short. All the doctors and assistants were very pleasant. I had an appointment with Dr. Choi, and although I saw him for only a few minutes, he made me feel very comfortable.” – Yasmeen A.
SCHEDULE AN APPOINTMENT
If you would like to learn more about Glaucoma Treatment call +1 (209) 239-5303 to make an appointment at Central Valley Eye Medical Group.
Testing For Glaucoma
The gold standard for functional glaucoma testing involves computer-automated visual field testing (perimetry). These visual field tests help a physician identify and manage worsening peripheral vision. The tests have high variability and require a physician to have a trained eye to help identify early subtle changes. Additionally, not all visual field tests are created equal. Depending on the patient, visual field tests need to be tailored and customized to ensure that ongoing visual field loss is caught in a timely fashion.
Imaging tests for glaucoma traditionally involved yearly photographs of the optic nerve to monitor for changes. Newer optical coherence tomography (OCT) allows for additional precision in monitoring for changes that a photograph could not catch. These scanners measure changes at the level of microns which is a unit of measurement 1/1000th the size of a single millimeter. Similar to visual fields, OCT results can be subtle and a comprehensive understanding of the complex data is imperative to accurately assess for glaucoma.
Laser Treatment for Glaucoma
There are many different types of laser treatments for glaucoma. The decision to advance treatment to laser therapy is a personal one and needs to be customized to each individual patient.
There are three main types of laser treatments used in glaucoma:
- Selective Laser Trabeculoplasty (SLT): A low-energy laser that is focused at the drain of the eye (trabecular meshwork) to help increase outflow and subsequently lower eye pressure.
- Laser Peripheral Iridotomy (LPI): A laser that is used to create a small opening in the peripheral iris to help decrease the risk of an acute angle closure attack.
- Micropulse Cyclophotocoagulation: A thermal laser is applied through the sclera of the eye and absorbed by the tissue that creates fluid within the eye (ciliary body). This lowers fluid production inside the eye and subsequently lowers eye pressure.
Minimally Invasive Glaucoma Surgery
Minimally invasive glaucoma surgeries (MIGS) is a group of glaucoma surgeries that help lower a patient’s eye pressure while not subjecting them to all the risks and side effects of traditional glaucoma filtering surgery. In general, to be termed “minimally invasive” a specific glaucoma surgery should have the following:
- If an incision is required, it should be micro-incisional and typically through the cornea.
- Minimal trauma to normal anatomy and physiology
- Reliable lowering of eye pressure.
- High safety profile (low side effects and risk of complications)
- Rapid post-op recovery, with minimal need for follow-up
There are many different types of MIGS procedures and studies are still ongoing on many of them. In general, your glaucoma specialist will evaluate if you are a good candidate for a MIGS procedure.
Glaucoma Filtering Surgery
Traditional glaucoma filtering surgery typically involves the creation of a hole in the wall of the eye (trabeculectomy) or placing a tube (tube shunt) inside the eye. These surgeries help to lower the pressure in the eye (and control glaucoma) by draining the fluid from within the eye to the outside of the eye. Although traditional glaucoma surgery represents the most invasive treatment for glaucoma, it also provides the greatest pressure lowering of all the treatment options.
Glaucoma Eye Drops
Another glaucoma treatment comes in the form of eye drops. These eye drops can do one of two things, depending on your situation and what you need. They can either increase the amount of fluid being created in your eyes or lower it, which can help regulate the pressure in your eyes. This treatment may cause temporary blurred vision and irritation.
What Are the Early Signs of Glaucoma?
Early signs of glaucoma are often subtle and can include:
- Blurred or narrowed vision
- Eye pain
- Halos around lights
Many people, however, experience no noticeable symptoms in the early stages. This is why regular eye exams are so important. Early detection allows for more effective treatment and helps prevent long-term vision loss.

Can I Prevent Glaucoma With Lifestyle Changes?
Lifestyle changes can help manage and reduce glaucoma risk. However, they may not prevent it entirely. Here are some steps you can take:
- Maintaining a balanced diet rich in antioxidants
- Exercising regularly to improve blood flow
- Managing stress
- Avoiding smoking
- Protecting eyes from UV exposure
- Staying hydrated
Regular eye exams are also crucial. They allow for early detection even when lifestyle factors are optimal.
How Often Should I Get Glaucoma Screenings?
The American Academy of Ophthalmology recommends adults undergo a baseline comprehensive eye evaluation at age 40.
Many people, however, experience no noticeable symptoms in the early stages. This is why regular eye exams are so important. Early detection allows for more effective treatment and helps prevent long-term vision loss.
What Are the Risks of Untreated Glaucoma?
Untreated glaucoma can contribute to progressive and irreversible vision loss. As the disease advances, peripheral vision gradually diminishes. This can potentially lead to tunnel vision and, eventually, complete blindness.
Glaucoma often develops without symptoms in its early stages. Because of this, many people don’t realize they have it until significant vision is lost. Timely diagnosis and treatment are essential for preserving eyesight and preventing further deterioration.
Is Glaucoma Hereditary?
Yes, glaucoma can have a hereditary component. A family history of glaucoma increases the risk. This is particularly true for primary open-angle glaucoma, the most common type.
Genetic factors play a role in eye pressure regulation and optic nerve health. These are crucial in glaucoma development.
If close relatives have had glaucoma, it’s wise to undergo regular screenings. You should also notify your eye care provider about your family history for early monitoring and preventive care.
How Does Glaucoma Affect Night Vision?
Glaucoma can significantly impact night vision, especially as peripheral vision loss progresses. People with glaucoma may:
- Find it difficult to adjust to low-light environments
- See halos around lights
- Experience reduced contrast sensitivity
All of these issues can make navigating in dimly lit settings challenging. These night vision issues tend to develop subtly and worsen as the condition progresses. This makes early detection and treatment crucial for preserving as much visual function as possible.
Why Choose Central Valley Eye Medical Group?
Choose Central Valley Eye Medical Group for top-tier, comprehensive eye care provided by board-certified ophthalmologists with advanced fellowship training.
Our expert physicians not only excel in patient care but are also dedicated educators. They actively teach residents about ophthalmic surgery, ocular anatomy, and ophthalmic medicine.
Recognized as thought leaders in the field, our doctors often contribute to respected ophthalmology resources relied upon by physicians worldwide. With this extensive expertise, Central Valley Eye delivers exceptional, informed care to enhance and protect your vision at every stage.
Schedule an Appointment Today!
At Central Valley Eye Medical Group, Inc, we value each individual patient and believe you deserve the best treatment possible. With state-of-the-art technology and equipment, we strive to provide you with the best service and results and make sure you feel warm and welcome within our office.
We are excited to help you begin your journey to a healthier and happier you. If you’re interested in glaucoma treatment, give us a call at +1 (800) 244-9907 to see what we can do for you. You can visit one of our three offices located in Stockton, Manteca, and Modesto, California.