SCHEDULE AN APPOINTMENT
If you would like to learn more about Diabetic Eye Care in Stockton, Modesto, & Manteca, CA call +1 (800) 244-9907 to make an appointment at Central Valley Eye Medical Group.
Diabetes is a disease that affects blood vessels throughout the body, particularly vessels in the kidneys and eyes. Patients with diabetes are at a higher risk of developing eye conditions as a complication of their disease. Diabetic-related eye problems develop from high blood sugar levels, which can cause damage to blood vessels. When diabetes affects the blood vessels in the eyes, it is called diabetic retinopathy.
What is Diabetic Retinopathy?
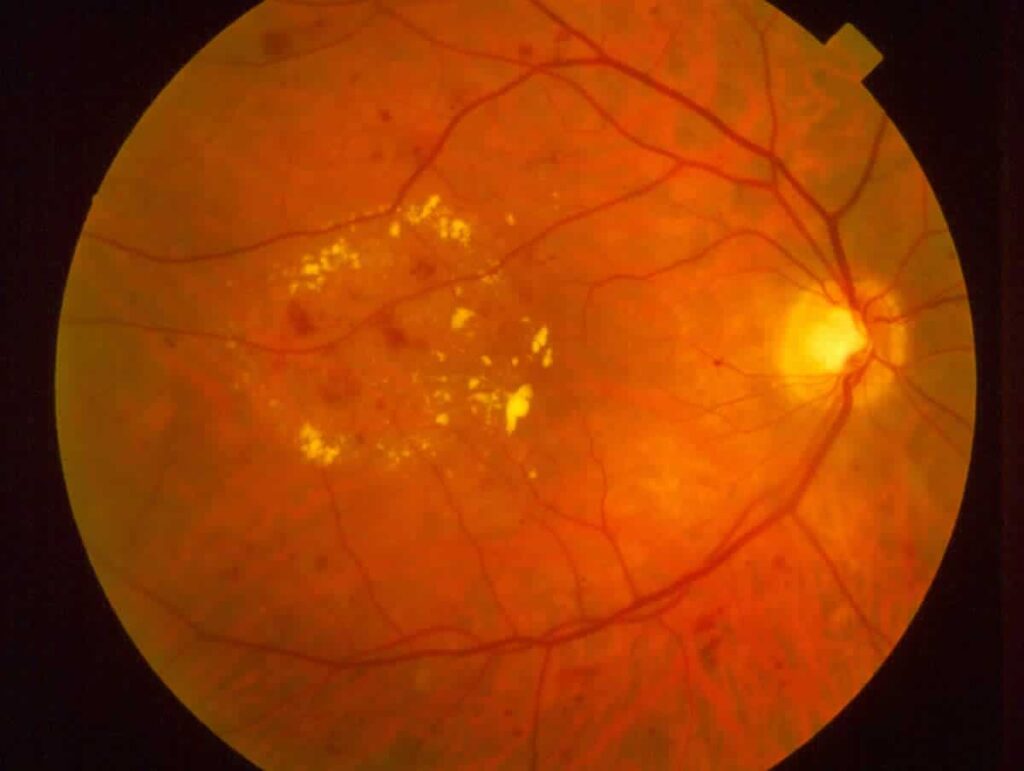
Diabetic retinopathy is a complication of diabetes. The longer a person has diabetes the higher the chance they will develop diabetic retinopathy. Diabetic retinopathy is the most common diabetic eye complication and specifically affects the blood vessels in the retina. The retina, located in the back of the eye, detects visual images and transmits them to the brain. When diabetes damages the retinal blood vessels they weaken, swell and leak. This results in a loss of vision and the ability to detect and transmit images. More than 40% of diabetics in the United States have some form of diabetic retinopathy which is the leading cause of blindness in America adults.
As diabetic retinopathy develops new blood vessels grow, these new vessels are your body’s attempt to overcome and replace the vessels that have been damaged by diabetes. However, these new vessels are not normal and may bleed, cause the vision to become hazy, and occasionally result in a complete loss of vision. In addition, abnormal blood vessels on the iris can lead to glaucoma and diabetic retinopathy can also cause the formation of cataracts.
Diabetic Retinopathy Symptoms
If symptoms do appear they can present as:
- Blurred or double vision
- Seeing flashing lights, blank spots or dark floaters
- Pain or pressure in either or both eyes
- Problems with peripheral vision
- Severe vision loss if left untreated
- Irreversible blindness in advanced stages
What Causes Diabetic Eye Disease?
Chronic high blood sugar levels caused by diabetes are the cause of diabetic retinopathy. These high levels damage the tiny blood vessels in the retina, which is located on the back of the eye. These blood vessels become blocked. To compensate, the eye grows new blood vessels, but they don’t develop normally and can begin to leak. This distorts the patient’s vision. As the condition progresses, these abnormal blood vessels proliferate on the surface of the retina. This can lead to scarring and cell loss in the retina.
Who Is Likely To Get Diabetic Retinopathy?
If you have diabetes, you can develop diabetic retinopathy. It generally won’t develop, however, until a person has had diabetes for at least a decade. These factors increase your risk:
- Longer duration having diabetes
- Poor control of your blood sugar levels
- High cholesterol
- High blood pressure
- Pregnancy
- Tobacco use
- Being African American, Hispanic, or Native American
Diabetic Retinopathy Treatment at Central Valley Eye Medical Group
The best treatment is early diagnosis. Otherwise, vision damage may already have occurred. Treatment depends on if you have nonproliferative (early stage) or proliferative (advanced) diabetic retinopathy. In early stages, simply managing your blood sugar effectively can slow the progression of diabetic retinopathy.
For decades, the main treatment for diabetic retinopathy, particular in the proliferative stage, was scatter laser surgery. Recently, new drugs have been developed and are proving to be effective for stopping the blood vessel development and decreasing fluid buildup of macular edema.These are the treatments used to treat diabetic retinopathy:
- Anti-VEGF injection therapy — In this treatment, drugs are used to block a protein called vascular endothelial growth factor (VEGF), which stimulates the growth of the abnormal blood vessels. The drugs are injected into the vitreous gel of the eye. These drugs have proven to be effective for reversing abnormal blood vessel development and decreasing fluid in the eye. Brand names are Avastin, Lucentis, and Eylea.
- Focal laser treatment — In this procedure, laser energy is used to either stop or slow the leakage of blood and fluid in the eye. Also called photocoagulation, laser burns close the leaking vessels. This laser surgery may involve just a few small laser burns or up to hundreds, depending on the patient’s condition.
- Scatter laser treatment — Also known as pan-retinal photocoagulation, here the areas of the retina away from the macula are treated with 1,000 to 2,000 tiny scattered laser burns. These burns cause new abnormal blood vessels to shrink and scar. Scatter laser surgery works best before new, fragile blood vessels have started to bleed.
- Vitrectomy — This surgical procedure is used to treat severe bleeding into the vitreous. In the procedure, a tiny incision is made in your eye to remove blood from the vitreous, as well as the scar tissue that is pulling on the retina creating detachment.
- These surgeries are very successful in preventing blindness in most people with diabetic retinopathy. Additionally, if your body has cataracts due to diabetic retinopathy, we can correct them with cataract surgery.
Schedule A Consultation
If you are noticing symptoms of diabetic eye disease, contact Central Valley Eye Medical Group for a comprehensive eye exam. Fill out our form or call us at 1.800.244.9907 to schedule a consultation in Stockton or Manteca, CA.
FAQ
Winter can be particularly harsh on the eyes, as cold outdoor air and indoor heating can exacerbate dry eye symptoms. To manage winter dry eye effectively:
-
- Use a Humidifier: Increasing the humidity in your home or office can help prevent dry eyes. Aim for a humidity level between 30% and 50%.
- Stay Hydrated: Drinking plenty of water helps maintain healthy tear production.
- Wear Protective Eyewear: When outside, wear wraparound glasses or goggles to shield your eyes from cold wind and prevent moisture from evaporating.
- Avoid Direct Heat Sources: Sit as far away from heaters or fireplaces as possible, as they can dry out the air around you.
- Use Artificial Tears: Over-the-counter artificial tears can provide immediate relief from dry eye symptoms. Use them regularly throughout the day.
- Limit Screen Time: Prolonged screen time can reduce your blink rate, potentially worsening dry eye. Take frequent breaks using the 20-20-20 rule: Every 20 minutes, look at something 20 feet away for at least 20 seconds.
Yes, untreated dry eye can lead to more serious eye conditions. Chronic dry eye can cause damage to the cornea, the clear front surface of the eye, leading to scarring and vision impairment. It may also increase the risk of eye infections, as tears are essential for washing away debris and bacteria. In severe cases, dry eye can lead to chronic inflammation, further damaging the eye’s surface and impacting overall eye health. Therefore, it is crucial to seek treatment if you experience persistent dry eye symptoms to prevent potential complications.
Yes, children can experience dry eye, though it is less common than in adults. Factors such as screen time, environmental conditions, or underlying medical conditions can contribute to dry eye in children. The treatment approach for children is similar to that for adults but often requires greater attention to the child’s comfort and ability to follow treatment routines.
Evaporative dry eye occurs when tears evaporate too quickly, often due to problems with the meibomian glands that produce the protective oil layer of the tear film. Without enough oil, tears break up rapidly, leaving the eye surface exposed and irritated.
Aqueous-deficient dry eye, on the other hand, happens when the lacrimal glands do not produce enough watery tears to properly lubricate the eyes.
Some patients experience a combination of both types.
Yes, allergies can significantly worsen dry eye symptoms. When the eyes react to allergens like pollen, dust, or pet dander, they release inflammatory chemicals that increase redness, itching, and irritation. This inflammation can destabilize the tear film, leading to tears evaporating more quickly. Additionally, frequent eye rubbing may further irritate the eye's surface.
Managing both allergy triggers and underlying dry eye disease is often necessary to reduce discomfort and maintain clearer, more comfortable vision.
Meibomian gland dysfunction (MGD) is one of the most common causes of evaporative dry eye. The meibomian glands, located along the eyelid margins, produce the oil layer of the tear film. This oil prevents tears from evaporating too quickly.
When these glands become blocked, inflamed, or produce poor-quality oil, the tear film becomes unstable. As a result, patients may experience burning, fluctuating vision, redness, and a gritty sensation.
Treating MGD through targeted therapies can improve tear stability and reduce chronic dry eye symptoms.
Dry eye can contribute to headaches and eye fatigue, particularly during prolonged reading or screen use.
When the tear film is unstable, vision may fluctuate, forcing the eye muscles to work harder to maintain focus. This added strain can lead to discomfort around the eyes, tension in the forehead or temples, and overall fatigue. Many people also blink less frequently while using digital devices, worsening dryness and increasing strain.
Addressing underlying dry eye disease often reduces associated headaches and improves visual comfort during daily activities.
The timeline for improvement depends on the type and severity of dry eye, as well as the treatment used.
Artificial tears may provide immediate, short-term relief. Prescription anti-inflammatory drops, such as cyclosporine-based medications, may take several weeks to reduce inflammation and improve natural tear production. Procedures like punctal plugs or IPL therapy may also require multiple sessions before full benefits are noticeable.
Because dry eye is often a chronic condition, consistent use of prescribed treatments is important. Many patients begin noticing gradual improvement within a few weeks of starting therapy.
Schedule A Consultation
If you suffer from dry eye disease, contact Central Valley Eye Medical Group to learn about treatment options. Call us at +1 (209) 239-5303 to schedule your consultation. We serve Stockton, Manteca, and surrounding areas.