Eyelid Malpositions
What is Ectropion?
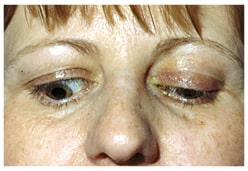
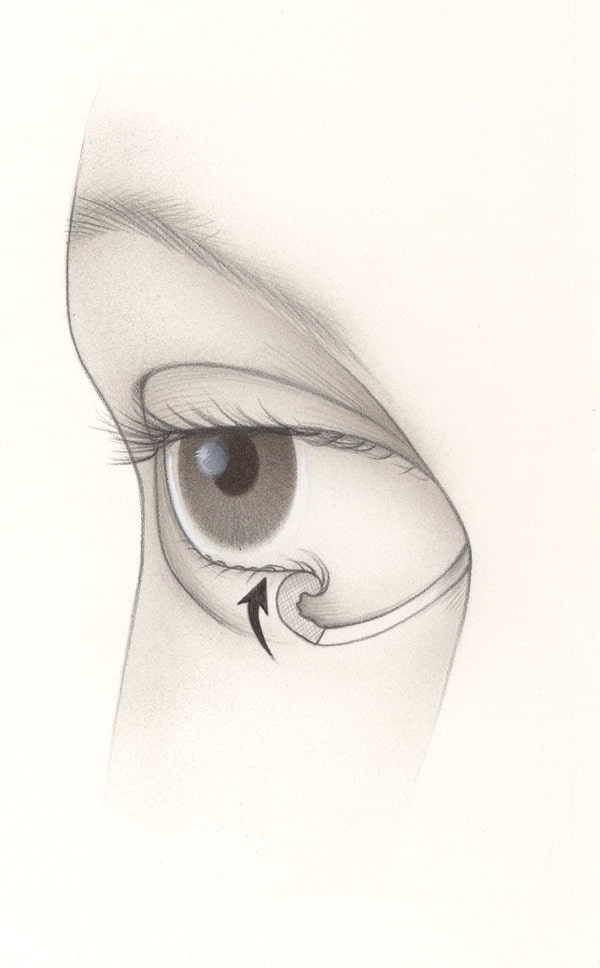
Ectropion is an eyelid malposition in which the lower eyelid turns outward and does not touch the eye. Consequently, the conjunctiva can become exposed and red. Ectropion usually affects one or both of the lower eyelids and rarely the upper eyelids.
Causes of Ectropion
Ectropion usually results from relaxation of eyelid tissues due to aging changes. It can also occur because of undetected skin cancers that pull down the eyelid. Other causes of ectropion include trauma, contraction of scar tissue of the surrounding skin, and eyelid or facial surgery. It may also occur congenitally or secondary to facial nerve palsy. The condition may be worsened by constantly wiping the eyes. Eyelid burns or skin disease may also result in ectropion.
Ectropion Symptoms
Many symptoms of ectropion are a result of chronic irritation of the eye and eyelid. Such symptoms include excessive tearing, crusting of the eyelid and mucus discharge, infection, corneal irritation, sagging skin around the eye, impaired vision, redness and pain of the eye, and sensitivity to light and wind. Ectropion may also result in poor drainage of tears through the nasolacrimal system. Also, the exposed inner lining of the eyelid becomes dry and inflamed, and the eye may be damaged.
Ectropion Treatment
Artificial tears and lubricating ointments can be used to moisten the cornea to prevent dryness of the cornea. When ectropion is caused by stretching of the eyelid’s supporting structures, surgery is the best treatment to repair the involved muscle and tendons of the eyelid. Depending on the cause of ectropion, surgery can be used to reposition the eyelid back to its normal position against the eye.
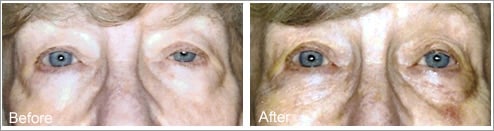
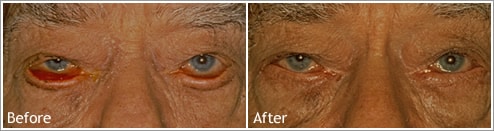
Ectropion Repair Before and After Photos
What is Entropion?
Entropion is an eyelid malposition in which the lower eyelid and eyelashes turn inward towards the eye causing the eyelid and lashes to rub against the cornea and conjunctiva.
Causes of Entropion
Entropion usually results from relaxation of eyelid tissues due to aging changes. It may also be due to infection or scarring on the inner surface of the eyelid, eyelid injuries, or tumors. Entropion may also be congenital if the eyelids do not form normally.
Symptoms of Entropion
Many symptoms of entropion are a result of chronic irritation of the eye and eyelid. Such symptoms include excessive tearing, crusting of the eyelid and mucus discharge, corneal irritation, sagging skin around the eye, impaired vision, redness and pain of the eye, sensitivity to light and wind, and foreign body sensation. Corneal infection and scarring may also occur as a result of entropion.
Entropion Treatment
Several surgical procedures may be used to tighten the eyelid and eyelid attachments thus restoring some of its elasticity and repositioning it normally. Alternatively, tape or sutures can be used to reposition the eyelid and protect the eye temporarily. Lubricating drops and ointments are also helpful. Medications may also be used to control eyelid inflammation or irritation and to treat scars. Sometimes scar removal and tissue grafts may be needed.
Ptosis Repair
What is Ptosis Repair?
Ptosis repair is the adjustment of the eyelid so as to improve eyelid drooping. The procedure may be required on one or both eyes depending on patient characteristics.
The excess skin in the upper eyelids can be removed surgically by a procedure called blepharoplasty. It improves side vision and other symptoms. Removal of the excess skin in either the upper or lower eyelids may improve appearance.
Symptoms of Ptosis
Ptosis may be congenital or acquired as a result of paralysis, neurogenic, trauma or aging. Classic signs characterized by drooping of the eyelid with or without levator disinsertion.
Drooping of eyelid may be constant or intermittent, or occur with use. In levator dehiscence, the ptosis is constant and worse in downgaze. In neurogenic ptosis, the defect may be at the level of the neuromuscular junction, the third cranial nerve nucleus or peripheral nerve or the sympathetic chain. In myasthenia gravis, the symptoms are variable and aggravated with use. The ptosis is constant without significant variation in patients with a third nerve palsy, Horner’s syndrome, or levator dehiscence.
Treatment for Ptosis
Depends on cause. Myasthenia gravis: oral prednisone with or without Mestinon. Always involve a neurologist before initiating therapy. Third nerve palsy: do strabismus surgery prior to considering ptosis repair to avoid symptomatic diplopia that requires patching. Complete third nerve palsy is difficult to manage; observation rather than surgical intervention is wise. Horner’s syndrome: internal conjunctival – Muller’s resection can be effective.
Neosynephrine drops can be used pre-operatively to help guide the selection of surgical approach. The posterior (conjunctival-Mueller’s excision) approach is only effective if Neosynephrine results in elevation of the eyelid to normal height.
Before and After Ptosis Surgery
 Ptosis Repair
Ptosis RepairWhat is Lagophthalmos?
Lagophthalmos (lag-ahf-thal-mus) is a condition in which the globe (eyeball) is not entirely covered when the eyelids are closed. It can be caused from a facial nerve (Bell’s) palsy, a protruding eye, or from eyelid retraction from Thyroid eye disease.
SCHEDULE AN APPOINTMENT
If you would like to learn more about Eyelid Malpositions call 1-800-244-9907 to make an appointment at Central Valley Eye Medical Group.


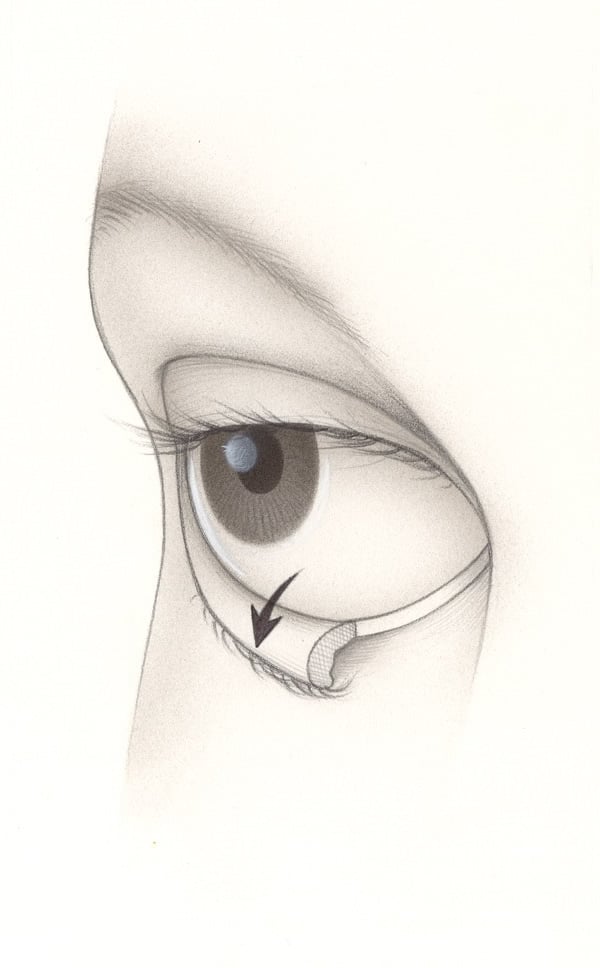
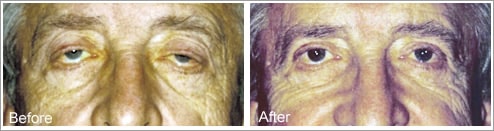 Bilateral Upper Eyelid Blepharoplasty & Ptosis Repair
Bilateral Upper Eyelid Blepharoplasty & Ptosis Repair